Creating Adjusted Scores Targeting mobiLity Empowerment (CASTLE 1): Determination of Normative Mobility Scores After Lower Limb Amputation for Each Year of Adulthood

Journal
Disability and Rehabilitation
READ ONLINE
Authors
Bretta L Fylstra1, Dwiesha L England1, Phillip M Stevens1,2, James H Campbell1, Shane R Wurdeman1,3
- Hanger Institute for Clinical Research and Education, Hanger Inc, Austin, TX, USA
- Department of Physical Medicine and Rehabilitation, University of Utah Health, Salt Lake City, UT, USA
- Department of Biomechanics, University of Nebraska at Omaha, Omaha, NE, USA
Background
As we shift towards value-based care, we need benchmarks to evaluate how well a patient is progressing. Normative mobility values specific to a patient’s age, amputation level, and cause of amputation provide patient-specific benchmarks for evaluating outcomes and moving towards value-based care. Additionally, expanding our understanding of these specific patient presentations to provide information that is more precise across every year of adulthood can assist with monitoring a patient’s trajectory and benchmarking performance for the majority of patients requiring lower limb prosthetic care.
The goal of this study was to establish mobility outcomes for each year of patients’ age for the primary causes of lower limb amputation: trauma and diabetes/dysvascular (DV). This analysis will facilitate a better understanding and potential to qualify what constitutes a good outcome by providing a normative mobility score specific to patients’ age and amputation level for trauma and DV. A secondary goal was to investigate how these mobility goals may change dependent on type of prosthesis provided to patients.
Objective
To create equations to calculate an expected mobility score for lower limb prosthesis users specific to their age, etiology, and amputation level to provide benchmarks to qualify good outcomes.
Design (n=29,522)
A total of 29,522 individuals (6,437 AKA and 23,085 BKA) met the inclusion criteria and were included in the final sample. A retrospective cross-sectional analysis of outcomes collected during clinical care was performed. Individuals were grouped based on amputation level (unilateral above-knee (AKA) or below-knee (BKA)) and etiology (trauma or diabetes/dysvascular (DV)). The mean mobility score (PLUS-M® T-score) for each year of age was calculated. AKAs were further stratified into having a microprocessor knee (MPK) or non-microprocessor (nMPK) for secondary analysis.
Results
Average mobility was calculated across age with respect to gender, amputation level, amputation cause, and device type. Overall, mobility declined with age, individuals who were male had higher mobility than those that were female, individuals with below-knee amputation had higher mobility than those with an above-knee amputation, and individuals with amputation due to trauma had higher mobility than those with diabetes/dysvascular disease. For individuals with an above-knee amputation, those with a microprocessor knee had higher mobility than those with a non-microprocessor knee.
FIGURE 1
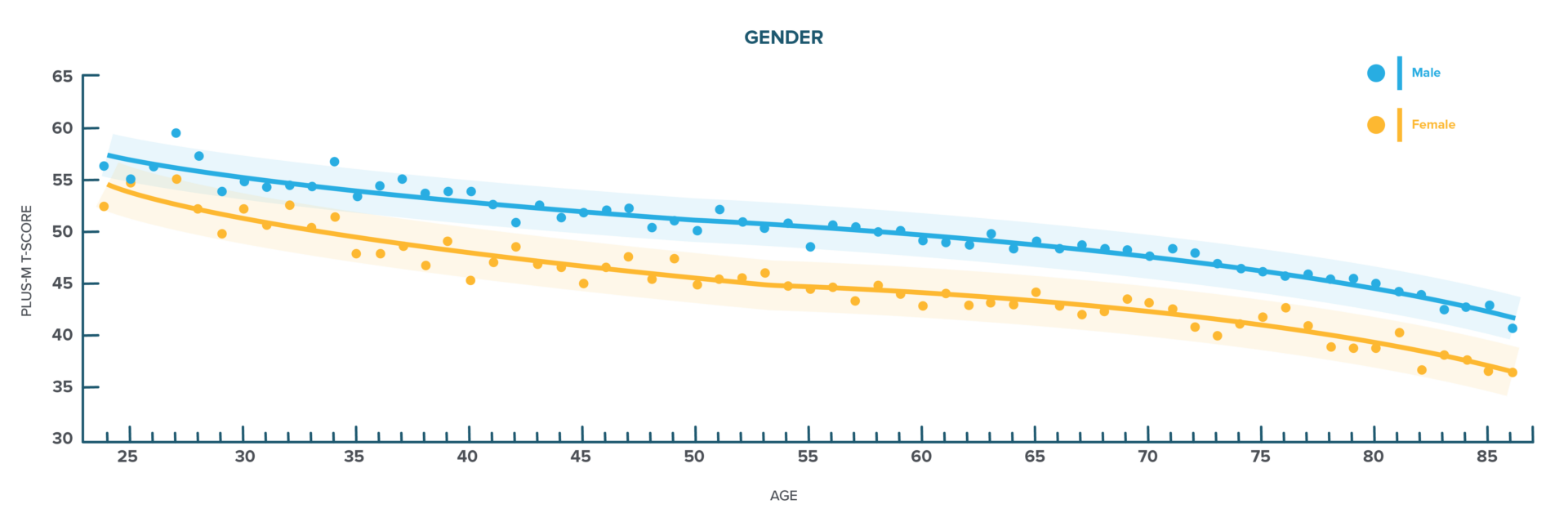
Age vs. Mobility across gender. Mobility decreases with age for both males and females. On average, males have higher mobility (PLUS-M) scores compared to females.
FIGURE 2
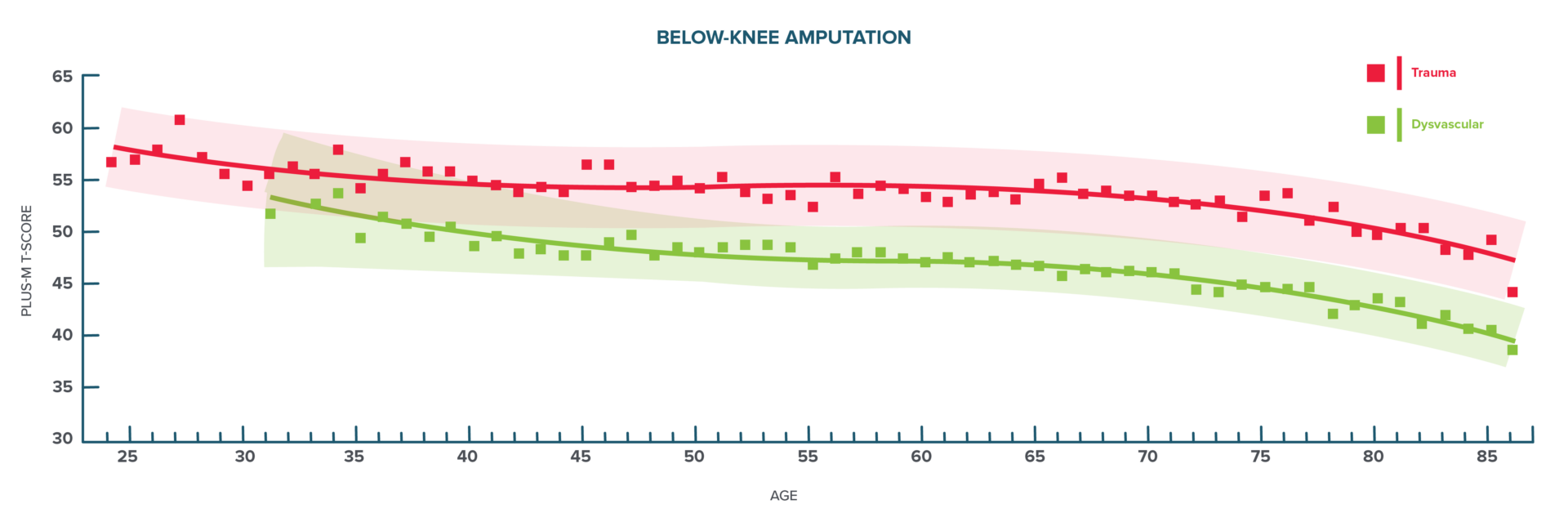
Age vs. Mobility for BKA. Mobility decreases with age for both trauma and DV etiologies. On average, trauma etiology has higher PLUS-M scores compared to DV.
FIGURE 3
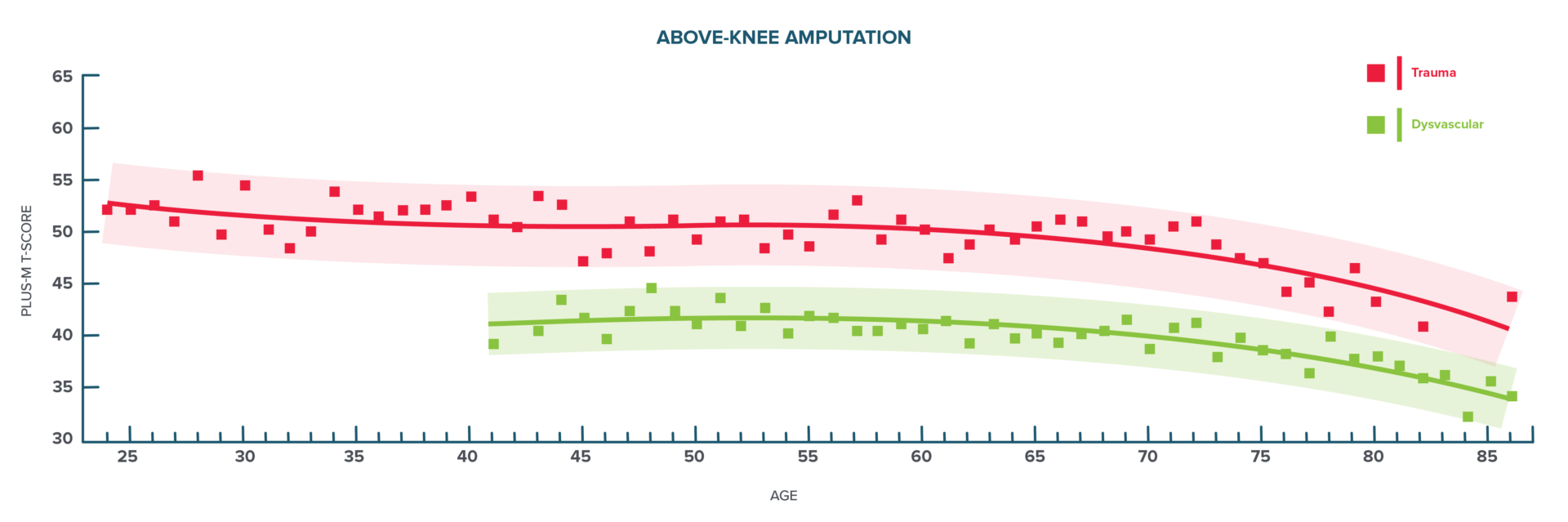
Age vs. Mobility for AKA. Mobility decreases with age for both trauma and DV etiologies. On average, trauma etiology has higher PLUS-M scores compared to DV.
FIGURE 4
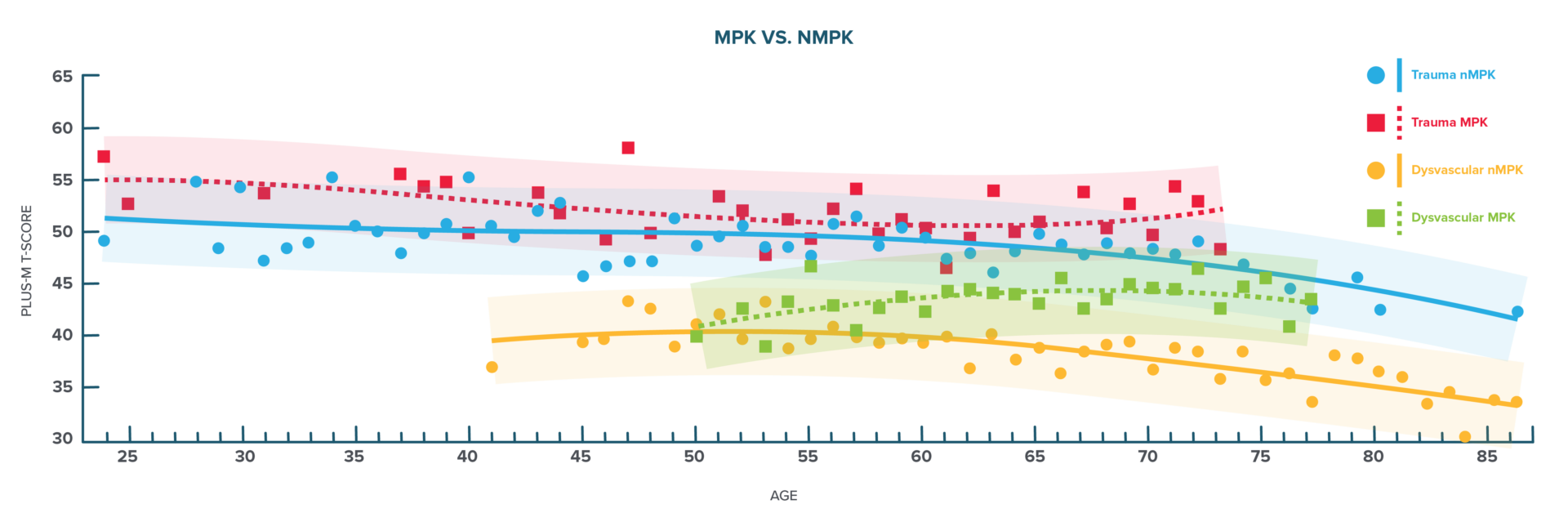
Age vs. Mobility for AKA stratified into MPK (filled markers and solid line) vs. nMPK (open markers and dashed line). For both trauma and DV, patients with an MPK have higher PLUS-M scores compared to those with a nMPK. Further, for patients with DV etiology, the MPK may slow the decrease in mobility relative to age.
Conclusion
- As expected, average prosthetic mobility declined with age. Overall, BKAs had higher mobility scores compared to AKAs and trauma etiologies had higher scores compared to DV. For AKAs, those with a MPK had higher mobility compared to those with a nMPK.
- The results of this study offer healthcare providers with tools for determining average mobility based on age and amputation level for the most common lower limb amputation etiologies of trauma and DV.
- It is reasonable to expect certain prosthetic devices, such as MPKs, may positively change the expected normative mobility scores for patients
Meet the Authors





More Published Research
This publication is just one of the studies conducted by the Hanger Institute for Clinical Research and Education, in collaboration with leading researchers, clinical, and academic institutions.
Latest Updates
Subscribe to stay up-to-date on our latest posts.


