GGEM: Gender, Geography, and EMployment Differences Based on Mobility Levels Among Lower Limb Prosthesis Users Living in the United States

Journal
Prosthetics and Orthotics International
READ ONLINE
Authors
Dwiesha L England, MSEng1, Taavy A Miller, PhD, CPO1,2, Phillip M. Stevens, MEd, CPO, FAAOP1,3, James H. Campbell, PhD, CO, FAAOP1, Shane R. Wurdeman, PhD, CP, FAAOP(D)1,4
- Hanger Institute for Clinical Research and Education, Hanger Clinic, Austin, TX
- Department of Public Health Sciences, University of North Carolina at Charlotte, Charlotte, NC
- Division of Physical Medicine and Rehabilitation, University of Utah, Salt Lake City, UT
- Department of Biomechanics, University of Nebraska at Omaha, Omaha, NE
Background
Lower limb amputation (LLA) can potentially have a major effect on a patient’s overall health, well-being, and functional mobility. Prediction of functional mobility outcomes after LLA is of concern to healthcare professionals given that a dramatic reduction in mobility can decrease quality of life, increase healthcare costs or utilization, or result in a decrease in occupational classification, including loss of employment.
Prosthetic rehabilitation aims to restore functional independence and provide patients with a mobility level similar to, or possibly greater than, their pre-amputation levels. Mobility restoration is one of the ultimate aims of rehabilitation among patients with LLA, and the relationship between gender, geography, employment, and functional mobility may be used by clinicians to make informed care decisions geared toward prosthetic selection and designed to maximize mobility.
Objective
To assess the relationship between gender, geography, and employment status on mobility among lower limb prosthesis users.
Design
A cross-sectional analysis of 7,524 patient mobility outcomes for unilateral prosthesis users across the United States was completed between January 1, 2017, and December 31, 2019. The regression model included the independent variables, such as age, gender, region, employment status, and amputation level. Mobility was entered as the dependent variable.
Independent Variables
The demographic variables included age, gender, region, employment status, and amputation level. Self-reported employment status (i.e., employed/student or unemployed), amputation level (i.e., above-the-knee or below-the-knee), and age (i.e., <65 or ≥65) were evaluated as dichotomous variables.
Dependent Variables
Functional mobility was measured through the Prosthetic Limb Users’ Survey of Mobility v1.2 (PLUS-M T-Score).
Results
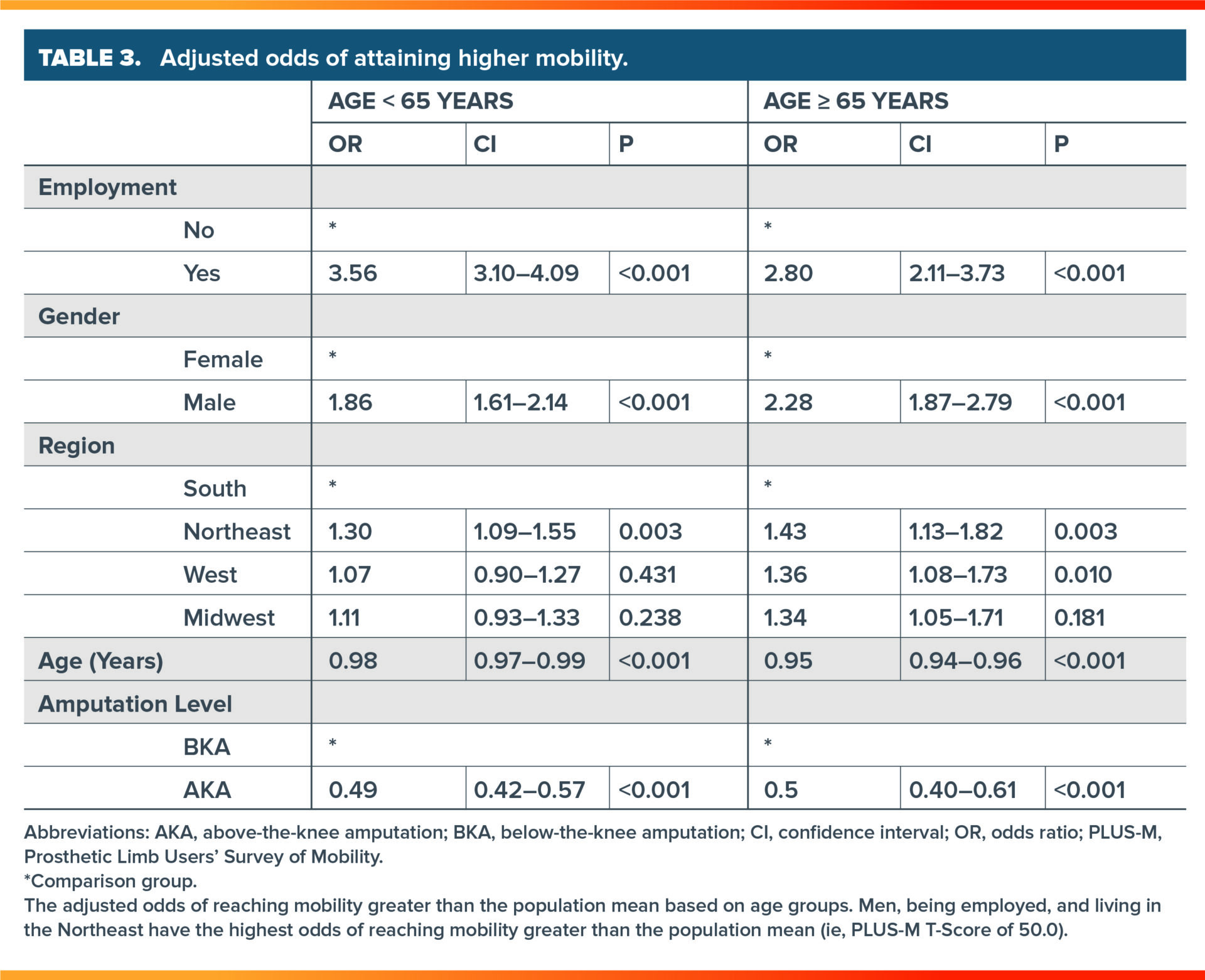
After controlling for age, gender, region, and amputation level, individuals who were employed had 3.6 times the odds of reaching above average prosthetic mobility levels (PLUS-M ≥ 50) than those unemployed (odds ratio 3.56, 95% confidence interval 3.10-4.09). Gender and geography were significantly associated with mobility as well. In comparison with men, women are less likely to ambulate, at above average mobility levels. In addition, individuals living in the South in the United States are less likely to achieve above average prosthetic mobility levels.
Conclusion
- This study provided notable advancements to the literature by updating findings on the relationship between current employment and mobility using a large sample size of patients representing the four regions in the United States. Unlike previous studies, the current study was not restricted to veterans and younger patients.
- Gender, geography, and employment are all factors that are highly associated with prosthetic users’ mobility. Being unemployed is associated with lower mobility levels, a finding observed for those both above and below the age of 65 years. These findings should be considered when developing targeted prosthetic rehabilitation plans.
- After amputation, a prosthesis can maximize mobility and may allow individuals with employment requiring physical activities to retain their occupation and, most importantly, their financial independence. All factors that may lend themselves to reduce mortality.
Meet the Authors





More Published Research
This publication is just one of the studies conducted by the Hanger Institute for Clinical Research and Education, in collaboration with leading researchers, clinical, and academic institutions.
Latest Updates
Subscribe to stay up-to-date on our latest posts.


