MAAT VII: Normative Mobility Values for Lower Limb Prosthesis Users of Varying Age, Etiology, and Amputation Level

Journal
American Journal of Physical Medicine & Rehabilitation
Read Online
Download Now
Authors
Dwiesha L. England, MSEng1, Taavy A. Miller, PhD1,2, Phillip M. Stevens, MEd1,3, James H. Campbell, PhD1, Shane R. Wurdeman, PhD1,4
- Department of Clinical and Scientific Affairs, Hanger Clinic, Austin, TX
- Department of Public Health Sciences, University of North Carolina at Charlotte, Charlotte, NC
- School of Medicine, University of Utah, Salt Lake City, UT
- Department of Biomechanics, University of Nebraska at Omaha, Omaha, NE
Background
As the seventh and final study in the Mobility Analysis of Amputees (MAAT) series, MAAT VII: Normative Mobility Values for Lower Limb Prosthesis Users of Varying Age, Etiology, and Amputation Level analyzed data from nearly 12,000 lower limb prosthesis users, who were grouped by age, amputation etiology, and above vs. below-knee amputation. MAAT VII established normative values for each group, ultimately expanding known benchmarks from two etiologies across four age groups, to four etiologies (cancer, congenital, trauma, and diabetes/dysvascular) across seven age groups. The awareness of differences across amputation etiologies extending across the lifespan of ages can assist the goal-setting process as part of prosthetic rehabilitation. Additionally, refined normative values provide the ability to benchmark new and innovative changes in clinical practice.
The MAAT series, which has been published regularly by the Hanger Institute for Clinical Research and Education since 2017, represents the largest national analyses of mobility among lower limb prosthetic users and clarifies the concept of prosthetic mobility as it relates to considerations such as satisfaction, quality of life, comorbid health conditions, and prosthetic component choices.
Objective
The objective of this study was to establish normative values for individuals with lower limb difference/amputation due to cancer or congenital etiologies, and expand those available for etiologies associated with trauma and diabetes/dysvascular.
Design
A retrospective cross-sectional observational analysis was performed on mobility outcomes completed in the United States.
Patient Inclusion Criteria:
- Data collected from April 2016-May 2019
- Adults aged 18 years or older
- Unilateral lower limb amputation (above-knee or below-knee) with prior experience using a prosthesis
- Reported etiology as either cancer, trauma, congenital, or diabetic/dysvascular disease
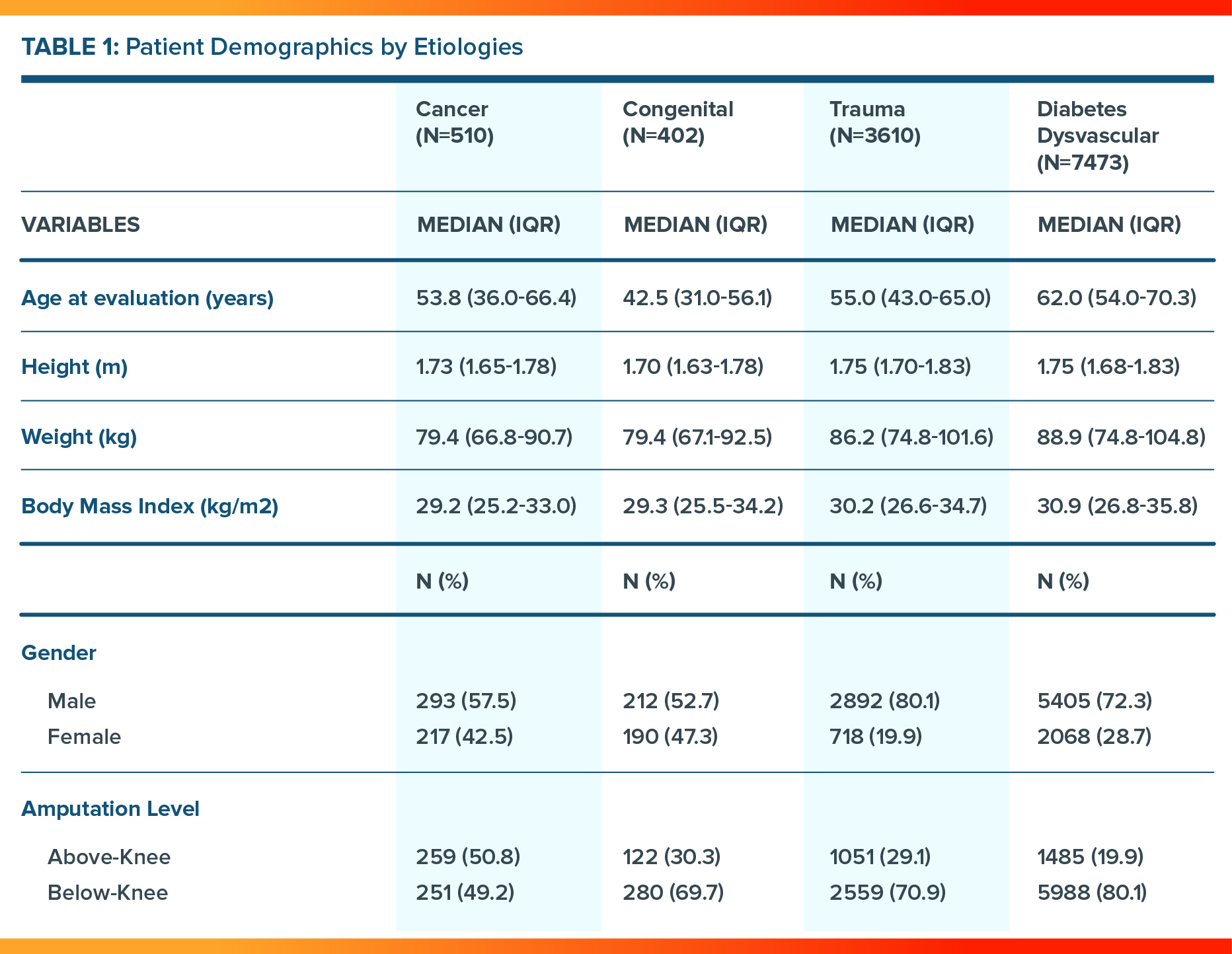
Table 1: Patient Demographics (n=11,995)
Results
Older individuals with above-knee or below-knee amputations reported reduced mobility across the four primary etiologies. As expected, the oldest age group had the lowest mobility across amputation level and etiology. The diabetes/dysvascular etiology had the lowest median mobility scores across amputation levels and was significantly different from trauma, cancer, and congenital disease.
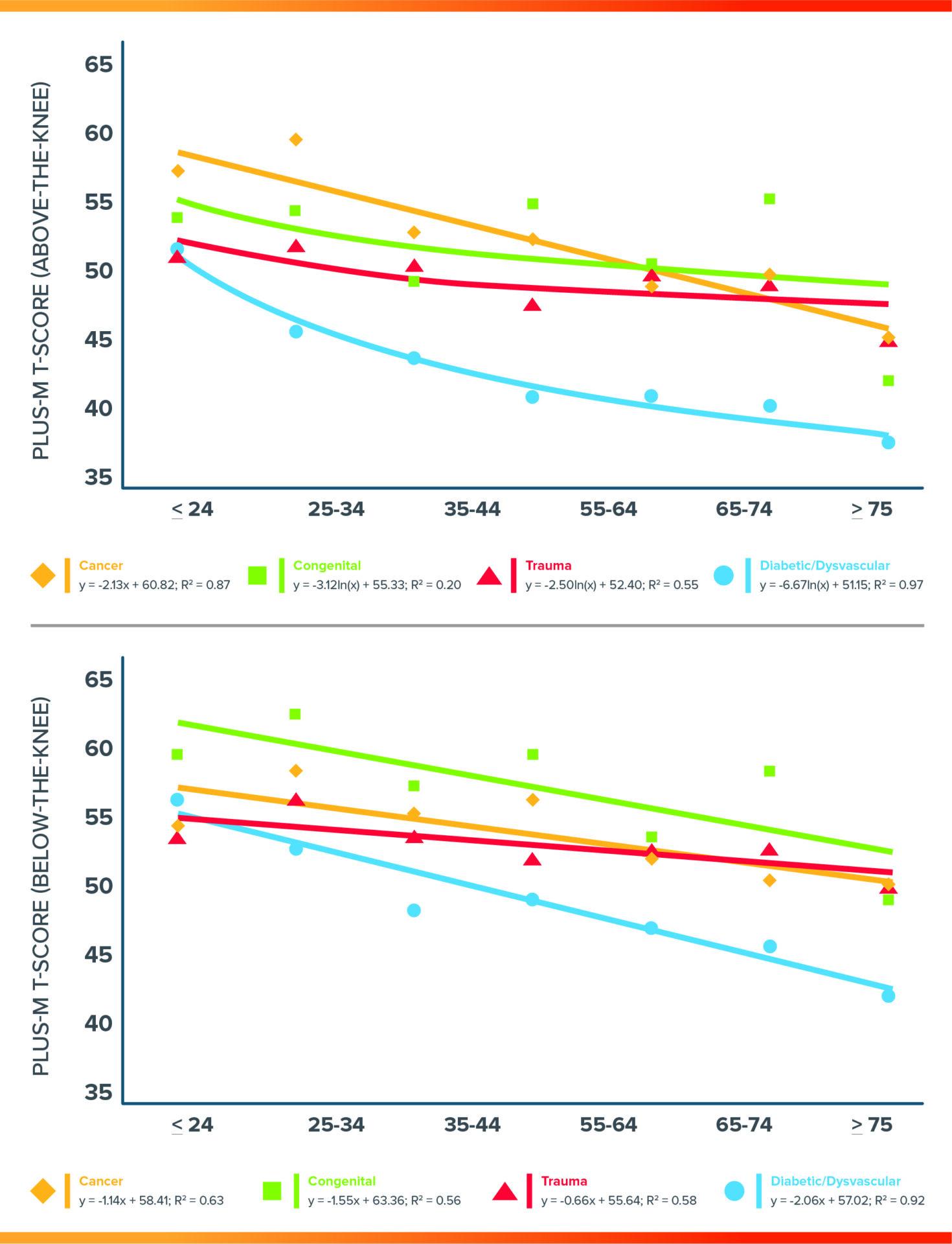
Figure 1
Changes in Mobility with Age
The optimal best fit line across age group medians was plotted for cancer, congenital, trauma, and diabetic/dysvascular etiologies for both individuals with above-the-knee and below-the-knee amputation. Diabetes/dysvascular shows the greatest decline with age.
Conclusion
- The findings of this study are valuable and insightful because mobility seems to decline at different rates across amputation levels for cancer, congenital, and trauma compared to diabetes/dysvascular.
- Individuals with amputation can struggle to understand realistic goal setting, which is also dependent on the underlying cause of amputation. Understanding the magnitude of the differences among the four etiologies may aid in the allocation of targeted interventions, and allows for a more nuanced discussion at the patient-clinician level for goal setting during the rehabilitation process.
- Clinicians can help patients set goals based on how well individuals that are similar to them are able to perform when achieving their highest reported mobility, subsequently preventing unrealistic goals as well as encouraging attainable goals.
- With an understanding of the general decline in mobility due to aging, future longitudinal studies may now have the ability to benchmark intervention performance in reducing the rate of decline in mobility associated with age.
Meet the MAAT VII Authors





The MAAT Series
The MAAT series has had an incredible impact on our profession over the last five years, advancing outcomes-based care and revolutionizing the way we leverage clinical research to discover best practices for our patients.
Latest Updates
Subscribe to stay up-to-date on our latest posts.


